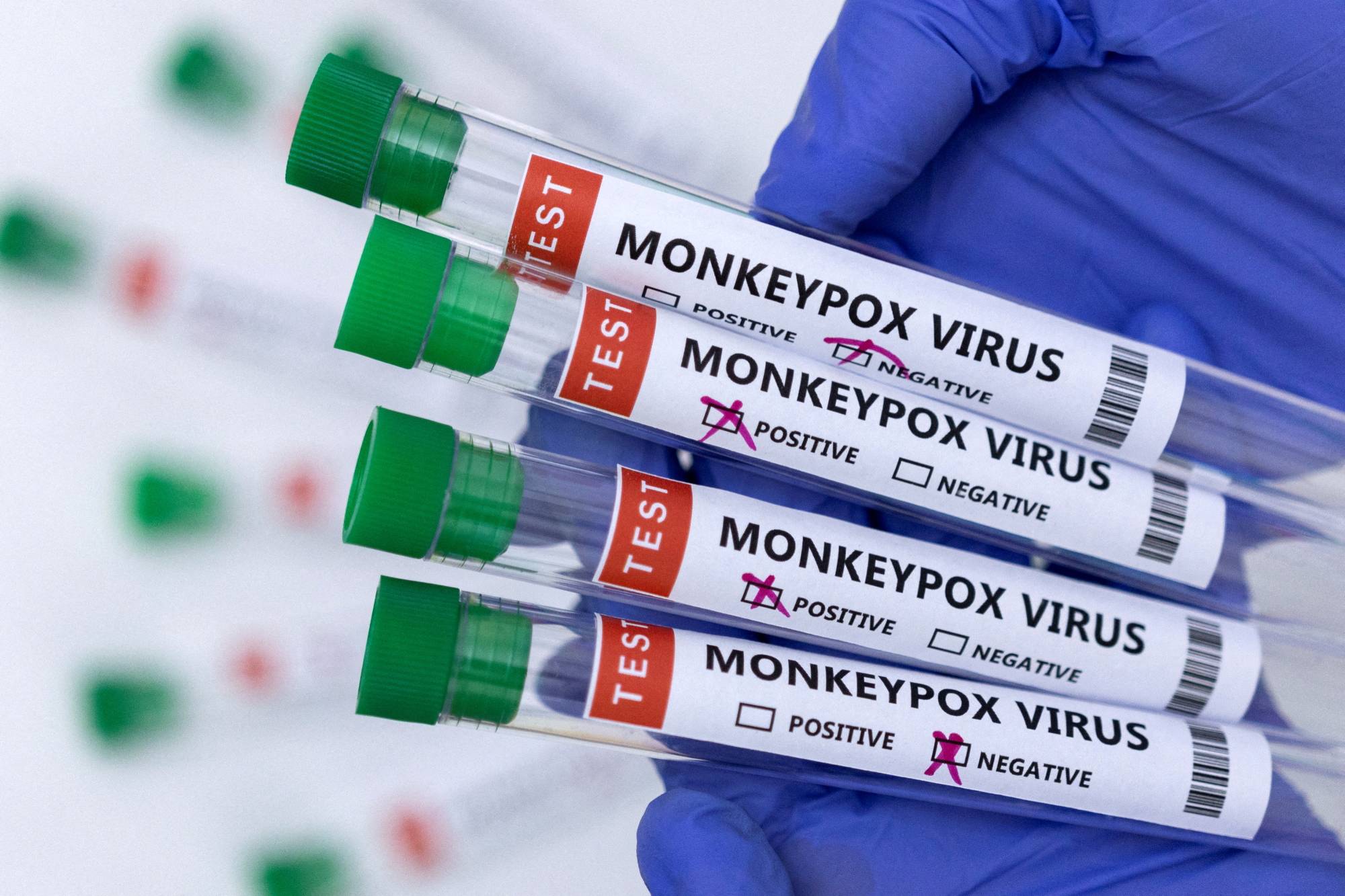
Recent News on Mpox
Mpox, previously known as monkeypox, has recently garnered significant attention due to an outbreak that began in 2022. The World Health Organization (WHO) declared it a Public Health Emergency of International Concern (PHEIC) due to its rapid spread across various countries. This outbreak has been characterized by an unusual number of cases outside the traditional endemic regions of Central and West Africa. The disease’s recent surge has led to heightened vigilance and research to understand its transmission and control measures better.
Transmission of Mpox
Mpox is primarily transmitted through direct contact with the blood, bodily fluids, or skin lesions of infected animals, particularly rodents and primates. Human-to-human transmission can occur through close contact with respiratory droplets, bodily fluids, or skin lesions of infected individuals. It can also spread via contaminated objects, such as bedding or clothing, used by an infected person.
Key transmission routes include:
- Direct Contact: Touching lesions or bodily fluids of infected individuals.
- Respiratory Droplets: Prolonged face-to-face contact with an infected person.
- Contaminated Objects: Handling items that have come into contact with the virus.
Signs and Symptoms
The symptoms of mpox typically manifest within 5 to 21 days following exposure. The disease progresses through a series of stages:
- Prodromal Stage: Initial symptoms often include fever, chills, headache, muscle aches, backache, and exhaustion.
- Skin Rash: A characteristic rash develops, starting with flat red spots that evolve into raised bumps and then into fluid-filled blisters. These blisters eventually crust over.
- Lymphadenopathy: Swelling of the lymph nodes, which can be seen in areas near the rash, is another distinguishing feature of mpox.
The rash usually appears on the face, hands, feet, and other parts of the body, including mucous membranes like the eyes, mouth, and genitals.
Investigations to be Done
Diagnosing mpox involves a combination of clinical assessment and laboratory tests. Given that mpox symptoms can be similar to other viral infections, accurate diagnosis is crucial. The primary investigations include:
- Polymerase Chain Reaction (PCR) Test: This test is used to detect the presence of the mpox virus’s DNA in skin lesions or other bodily fluids. It is the most definitive method for diagnosing mpox.
- Serological Testing: Blood tests to detect antibodies against the mpox virus can help in confirming recent or past infections.
- Virus Isolation: Culturing the virus from lesion samples can provide a definitive diagnosis, though this method is less commonly used due to the complexity and risk of handling.
- Immunohistochemistry: This technique uses antibodies to detect the presence of viral proteins in biopsy samples from skin lesions.
- Histopathological Examination: Microscopic examination of biopsy specimens from lesions can help identify characteristic features of mpox, such as intracytoplasmic inclusions.
- Differential Diagnosis: To rule out other conditions with similar presentations, such as varicella-zoster virus (chickenpox), smallpox, and other pox-like diseases, additional tests and evaluations might be necessary.
Early diagnosis and intervention are critical to managing mpox effectively and preventing its spread. Public health measures, including contact tracing, isolation of infected individuals, and vaccination where applicable, are essential components in controlling outbreaks.
As the situation evolves, staying informed through reliable sources and adhering to public health guidelines is crucial for both healthcare professionals and the public.